This year’s holiday season arrives as the flu, respiratory syncytial virus — RSV — and multiple strains of COVID-19 are circulating.
Sacramento County has high community COVID-19 transmission — a CDC metric meaning the county has at least 100 new cases per 10,000 people in the past 7 days — again, meaning holiday gatherings run the risk of being superspreader events. And anecdotal shortages of children’s cold and flu medicine along with filled pediatric hospitals can make it difficult to get speedy treatment for sick children.
“It’s still important to avoid catching COVID-19,” said Dr. Noha Aboelata from Roots Community Health Center in Oakland. “We’re learning more about the cumulative nature of the harms of repeat infection … people are catching COVID-19 and having strokes or heart attacks within the month following acute infection, even if that infection was mild.”
It’s not all grim — there are preventative measures you can take to make get-togethers safer without nixing them all together, Aboelata said.
Here’s some advice about how to reduce risk when coming together, along with where to get tests locally and how to respond if someone in your household gets sick after a party or gathering.
Layer preventative measures — use the swiss cheese model
Any mitigations are better than none, says infectious disease scientist Adam Moore, currently in an integrative pathobiology PhD program at UC Davis.
He and Aboelata recommended using the “Safer In-Person Gatherings Toolkit” from community organization People’s CDC as a resource for people to consult during event planning.
“It is absolutely meant to be a mix and match system,” Moore said. “The more layers you use, the better, but if you can’t use them all, that doesn’t mean you need to give up on the ones you can use.”
Make a contingency plan — and a guest list
Because it’s often difficult to coordinate treatment when you’re not feeling well, Aboelata suggests that people figure out how they might be able to access treatment, namely Paxlovid or Tamaflu, before any potential meet-up.
The California Department of Health has partnered with telehealth provider Sesame Care to provide free virtual COVID-19 visits for people with positive COVID-19 tests and symptoms to get prescribed Paxlovid. There are also several test-to-treat sites in Sacramento and throughout the state where you can get prescribed Paxlovid immediately after getting a positive COVID-19 test on-site.
Aboelata also recommends making a guest list, so if one person tests positive for COVID-19 or gets the flu or RSV, it’s easy to contact everyone who was present to let them know they’ve been exposed.
“You have to start your [COVID-19] treatment within five days, and so the sooner people know — especially vulnerable people and people who would be eligible for treatment, those are the folks that we worry a lot about — they can get tested and get treated,” she said.
Get the flu vaccine and the bivalent booster
With only 20% of the Californian population — which rises to almost 23% in Sacramento County — having received the bivalent booster, health officials are recommending people get the booster if eligible, especially since it’s effective against the current circulating strains of COVID-19.
“Vaccines help and they do work,” said Dr. Hakeem Adenyi, medical director at the Sacramento Native American Health Center. “If you haven’t been vaccinated against the flu, if you haven’t been vaccinated against COVID, please go out there and get it. It’s important that we continue to try to stem the tide because our hospital systems are really feeling the brunt of it.”
You can find a vaccine clinic near you or make an appointment at MyTurn.ca.gov or by calling the California COVID-19 Hotline at 833-422-4255 (Monday through Friday, 8 a.m.-8 p.m. Saturday and Sunday, 8 a.m.-5 p.m.).
The bivalent booster dose can be administered for those 5 and older at least two months following any COVID vaccine or monovalent booster dose.
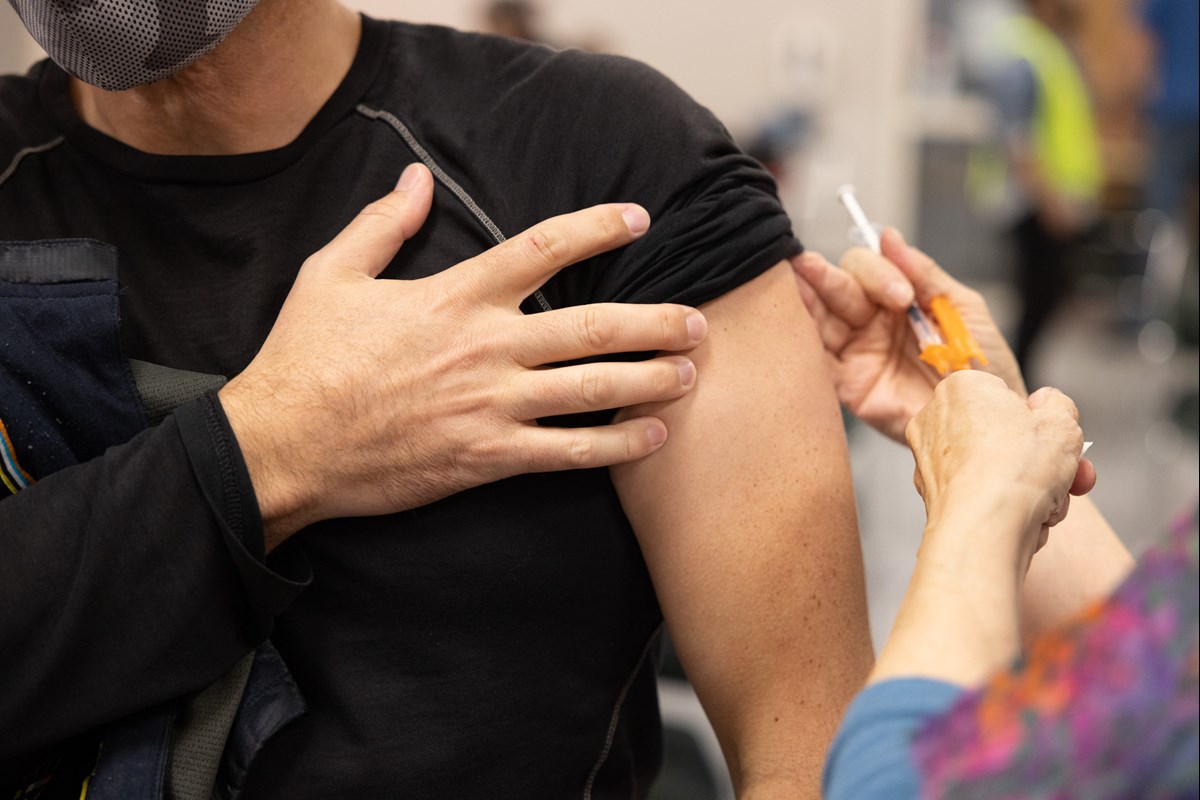 A vaccine clinic being held at the Pannell Center in Sacramento, Friday, Nov. 19, 2021.
A vaccine clinic being held at the Pannell Center in Sacramento, Friday, Nov. 19, 2021.Stay home if you have symptoms
Regardless of a negative COVID-19 test, professionals say that if you have symptoms, the best call is to stay home.
“It’s really important for people to keep in mind that one missed holiday season is a lot easier to deal with than this being someone’s last holiday season, because they gathered and someone got COVID-19 or flu or RSV, and it took a really dark turn for them,” Moore said. “All of these things can really mess you up.”
Plus, because flu and RSV have similar symptoms to COVID-19, one or multiple negative COVID-19 tests could still mean you have one or both of the other illnesses.
“Oftentimes, we look at getting the COVID test, and many of us feel like it’s a victory when it’s not COVID,” Adenyi said. “But if you’re not feeling well, it’s really important to find other ways to interact with friends and family [that aren’t in person].”
Get treatment like Paxlovid or Tamiflu, rest and hydrate if you’re sick
Aside from getting antiviral treatment like Paxlovid or Tamiflu that can shorten the course of COVID-19 or a flu, respectively, Adenyi from the Sacramento Native American Health Center stressed the importance of resting and hydrating if you end up getting sick after gathering.
“Rest is paramount,” he said. “We don’t sleep enough as a group … we need to listen to our bodies and take care of them, and rest is a key component of that.”
Rest has also been shown to reduce incidence of post-COVID incidents, or long COVID.
Mask up in indoor settings
Since the most dominant strains of COVID-19 tend to incubate 3-4 days before causing symptoms, one of the mitigations listed in the People’s CDC one-pager checklist for safer gatherings is to avoid unmasked indoor activities for the five days leading up to gathering in person, which can lead to greater pre-event COVID-19 test accuracy.
Masking isn’t just a COVID-19 precaution, said Kevin Sunga, a community health worker in Stockton. He’s the program director of the Equity in COVID and Health Outcomes team at Little Manila Rising and works closely with licensed health care professionals and local health jurisdictions.
“Masking up doesn’t just prevent from COVID, keeping COVID away,” he said. “It also helps protect against RSV and flu.”
Dr. Aimee Sisson with Yolo County Public Health also urged people to get the best-quality mask they can. Ranked from the most to least protective, would be a N95, then a KN95 or KF94, then a surgical mask and last, a cloth mask.
“We got trained with the surgical masks — we were using a new one every day,” Sisson said. “But with these higher-quality, KN95, N95, KF94 masks, you can stretch a mask out to work for a couple weeks.”
NPR has a guide on how (and where) to shop for good-quality masks and how to decontaminate them between uses.
For those who are traveling to gatherings, Aboelata also recommends wearing a high-quality mask the entire travel route.
If you have to take off your mask to eat or drink, she said it’s best to wait until after everyone’s finished eating their served meal, since people will largely have masks back on or won’t be talking as much.
Another bad time to unmask: When the plane is on the ground.
“Typically that’s a very high-risk time because the HVAC isn’t necessarily turned on and everyone is huffing and puffing walking up and down the aisles, so that’s when you really need that mask to be fitting well,” she added.
Test day-of if you only have a rapid test, or multiple times if possible
In Sacramento County, there are still places people can get COVID-19 tested for free.
And in Yolo County, Sisson said, there are a lot of places to get free antigen tests.
“Yolo County is giving them away at libraries, in vending machines,” she said. There are also other free testing locations throughout the county.
The USPS also restarted its free test program, and every household can place one free order containing four at-home COVID-19 tests, to be shipped the week of Dec. 19.
Insurance covers the cost of eight at-home COVID-19 tests a month. At CVS or Walgreens, you can provide your insurance information to place an online order for tests.
Hosts can also set up a testing station beforehand and wait the 15 or 20 minutes for a rapid test result to show, Aboelata suggested.
Plan for indoor-outdoor gatherings
While it is getting colder, meeting in person outdoors is still the safest option for a gathering, especially if you’re unmasking, Sisson said.
“If you have a heat source that you can take advantage of outdoors, like a fire pit or some heating element, that’s one option,” she said.
Another suggestion from Aboelata: Gatherings can also function with an indoor-outdoor model: Guests are masked for their time indoors, but go outdoors to unmask when eating and drinking.
Ventilate any indoor gatherings
Making sure there’s good airflow during indoor gatherings can be a way to reduce the amount of virus in the room, so if someone is contagious, less of the virus will remain in the room to infect others.
One easy way to ventilate is to open windows, health professionals say. Some, like Aboelata, also recommend getting a carbon dioxide monitor — since if the number is high and CO2 is accumulating, “other things are accumulating as well, like viruses.”
If it’s in your budget, you can also invest in air purifiers, get HEPA filters for your HVAC system or construct a lower-budget air purifier, called a Corsi-Rosenthal box, with a box fan, four MERV13 air filters and duct tape.
Correction: This story has been updated with the correct spelling of Dr. Noha Aboelata’s last name.