Jacqueline Garcia & Virginia Gaglianone, The USC Center for Health Journalism Collaborative
The case of 10-year-old Rosa María Hernández gained national attention in October 2017 when she was detained by immigration agents while traveling in an ambulance for medical treatment in Texas.
Hernández, who is physically and mentally disabled, needed emergency gallbladder surgery and was sent to a Corpus Christi hospital. On the way, the ambulance passed through an immigration checkpoint.
Even though Hernández was accompanied by an adult cousin who was a U.S. citizen, federal authorities followed the ambulance to the hospital. After the surgery, Hernández was held in a juvenile detention facility for more than a week before she was released to plead her case to stay in the country.
Such cases have become more common under the Trump administration’s tougher enforcement of immigration laws including a mass roundup of migrant families with deportation orders scheduled to start on June 23. That has sparked fear for undocumented immigrants who, in certain cases, avoid going to hospitals and health care centers for fear of being intercepted by Immigration and Customs Enforcement (ICE) agents.
To help immigrants contend with these difficult situations, a new set of practices has emerged within health clinics that serve large numbers of undocumented patients.
Immigration enforcement in hospitals is rare, but high-profile cases of such enforcement in or near hospitals, such as in Hernández's case, heighten fears in immigrant communities.
“We see the impact of this immigration-related stress, such as in the case of patients who avoid medical care because they are unsure if a hospital or clinic cooperates with immigration authorities, which can put them in danger,” said neurologist Altaf Saadi, a clinical instructor of medicine and member of UCLA’s National Clinician Scholars Program. “This means that, while immigration law enforcement in hospitals is rare, the fear is there, and it is affecting the behavior of patients.”
Sanctuary Clinics Offer Reassurance
Saadi has coined the terms “sanctuary doctoring,” “sanctuary hospitals” and “sanctuary clinics” to refer to special procedures adopted to shield those without legal status when they visit a doctor. The terminology is based on the religious concept of “sanctuary” that was adopted by cities and states to try to limit cooperation with federal immigration authorities.
"Just as there is no established legal definition of ‘sanctuary,’ there is no established definition of ‘sanctuary’ in the health care setting,” said Saadi.
In Los Angeles, several clinics and medical centers are known as offering “sanctuary” in their efforts to keep patient data confidential while providing health care.
One medical center that is open about its sanctuary status is the Monsignor Oscar A. Romero Clinic, with two locations, one in the MacArthur Park area and another in Boyle Heights: two areas with large numbers of residents originally from El Salvador, Guatemala and Mexico.
 Aurelia Ventura / La Opinión
Aurelia Ventura / La OpiniónThe Romero Clinic, as it is commonly known, declared its sanctuary policy after noticing an alarming increase in missed medical appointments since ICE raids began all over the country in early 2017.
An estimated 50% of patients receiving care at the Romero Clinic are undocumented, said Stephanie Lemus, director of patient services and community relations at the clinic.
Lemus explained their patient protection protocol: In the event of an ICE visit, the staff announce the agents’ presence by means of an unidentified code and immediately close the facility. Patients who could be targeted are moved from the reception area to other parts of the clinic restricted to staff.
A staff member is designated as a spokesperson to verify if ICE has a court order to arrest a specific person. In cases where ICE does have a court order, staff coordinate legal representation for the patient.
Lemus said that, so far, the developed protocol has not been used, but clinic staff are ready to act.
“Our mission is founded on protecting the Latino community, the most vulnerable among us, in the tradition of Monsignor Oscar Romero,” said Lemus, referring to the Salvadoran martyr who was beatified in 2018.
“For us it is important to protect our patients regardless of their immigration status, since our advocacy work is reflecting the mission of Monsignor Romero,” Lemus said.
Connie, 49, an undocumented immigrant from Mexico, became involved with the Romero Clinic two years ago as a health promoter. There, she learned about health services that otherwise would be beyond her financial means.
“At the clinic I get my (mammogram), checkups, laboratory tests,” said Connie, who did not provide her last name for safety reasons. “It's very important to me that the clinic provides these services, because sometimes people don't have the money for a physical exam that can cost up to $150.”
Connie said she has encouraged others to get health checkups at the clinic.
“I have friends who didn’t know they were sick. They were told they had diabetes or high blood pressure,” she said.
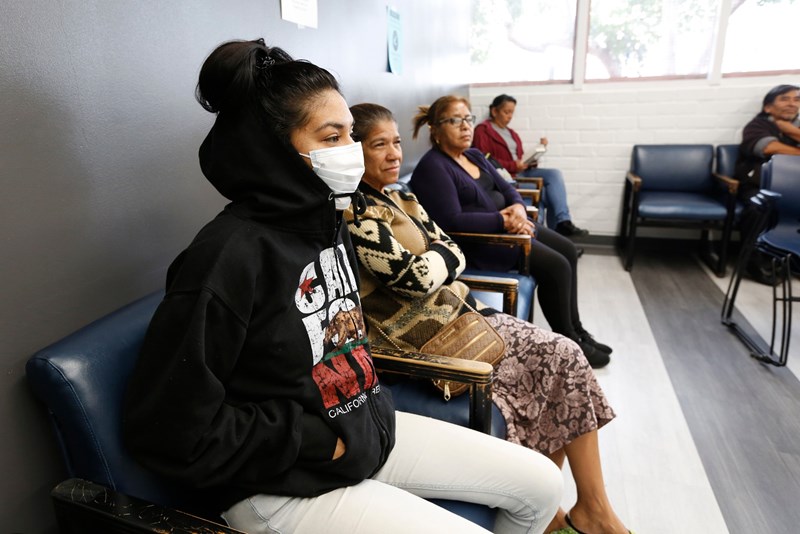 Aurelia Ventura / La Opinión
Aurelia Ventura / La OpiniónWhat Does ‘Sanctuary’ Mean
Saadi said she’s completing a study in several U.S. states exploring how clinics and hospitals apply the idea of “sanctuary” to welcome and protect immigrant patients.
“What I found was that there are many actions that a health center can take to make its facilities safer for immigrant patients, such as having a specific protocol on what to do if (ICE) show up at the health care center, or how to avoid identifying the patient's immigration status in their medical records,” explained Saadi.
While she doesn’t know exactly how many medical centers or doctors identify as part of the “sanctuary” network, she said California Senate Bill 54, which took effect in January 2018, requires all public health care facilities to implement policies that limit collaboration with immigration agents.
“Hospitals and clinics throughout Los Angeles County and California are working to implement these policies in accordance with SB 54,” she said.
The federal Emergency Medical Treatment and Labor Act (EMTALA), enacted in 1986, guarantees public access to emergency services, regardless of an individual’s ability to pay. And the Social Security Act imposes specific obligations on Medicare-participating hospitals that also offer emergency services.
Such hospitals are required to provide a medical screening for emergency medical conditions, including active labor, regardless of the patient's ability to pay.
Hospitals are also required to stabilize patients with an emergency medical condition. If a hospital cannot do that, or if the patient requests it, a transfer to another medical facility must be implemented.
Saadi said she wants to help health providers go beyond simply complying with the law for emergency treatment.
She said the term “sanctuary” expresses a general sentiment for doctors who want the best for their patients, regardless of their immigration status. That includes doctors who serve the social needs of immigrants, as well as their medical needs.
Still, Saadi admits that the sanctuary concept has its limits, given the ability of immigration agents to detain undocumented immigrants once they are outside the clinic or hospital.
“It is important not to provide a false sense of security with the use of this language,” she said.
 Aurelia Ventura / La Opinión
Aurelia Ventura / La Opinión
Follow us for more stories like this
CapRadio provides a trusted source of news because of you. As a nonprofit organization, donations from people like you sustain the journalism that allows us to discover stories that are important to our audience. If you believe in what we do and support our mission, please donate today.
Donate Today